[[[SUMMARY_START]]]
GLP-1 medicines have moved from diabetes care into the center of obesity treatment.
They can produce major weight loss and may lower risks tied to heart disease, sleep apnea and other conditions.
They also bring side effects, high costs, supply pressures and concerns about unapproved versions.
Scientists are still studying what happens after years of use and after patients stop treatment.
[[[SUMMARY_END]]]
GLP-1 drugs have become one of the biggest health and biotechnology stories of the decade. Once known mainly as diabetes medicines, they are now widely discussed as weight-loss treatments that can change appetite, body weight and long-term disease risk. Their rise has also raised difficult questions about safety, access, cost and how much remains unknown.
## How the medicines workGLP-1 stands for glucagon-like peptide-1. It is a hormone made in the gut after eating. It helps the body release insulin, slows how quickly the stomach empties and sends signals of fullness to the brain.
Modern GLP-1 medicines copy or strengthen that signal. Semaglutide is sold for diabetes and weight management under different brand names. Tirzepatide, used in diabetes and obesity treatment, acts on both GLP-1 and another hormone pathway called GIP. Newer pills are now joining the market, expanding a field that was first dominated by weekly injections.
The basic result is simple. Many patients feel less hungry. They may eat smaller portions. Over time, that can lead to large weight loss, especially when the medicine is used with nutrition changes and physical activity.
## The good: real weight loss and wider health benefits
Clinical trials have shown weight loss that was hard to reach with older medicines. In major studies, semaglutide helped many adults lose about 15% of body weight on average. Tirzepatide produced average losses near 21% at the highest tested dose in a large obesity trial.
Those numbers matter because even smaller weight reductions can improve blood pressure, blood sugar and cholesterol in some patients. For people with obesity-related disease, larger and sustained weight loss can be more than cosmetic. It can affect daily mobility, diabetes risk and heart health.
The benefits are no longer limited to the bathroom scale. Semaglutide has been approved in the United States to reduce the risk of major cardiovascular events in adults with established heart disease who also have obesity or overweight. Trial data showed a 20% relative reduction in the combined risk of cardiovascular death, heart attack or stroke in that group.
Tirzepatide has also gained an obesity-related sleep indication. It was approved for adults with obesity and moderate to severe obstructive sleep apnea, alongside diet and physical activity. That approval reflected growing evidence that weight loss can improve some forms of sleep-disordered breathing.
The drug technology is also moving quickly. Oral semaglutide for weight management was approved in late 2025. Eli Lilly’s oral GLP-1 drug orforglipron was approved in April 2026 for adults with obesity or certain adults with overweight. Pills may help people who do not want injections, although they still require medical supervision.
## The bad: side effects, cost and copycat risks
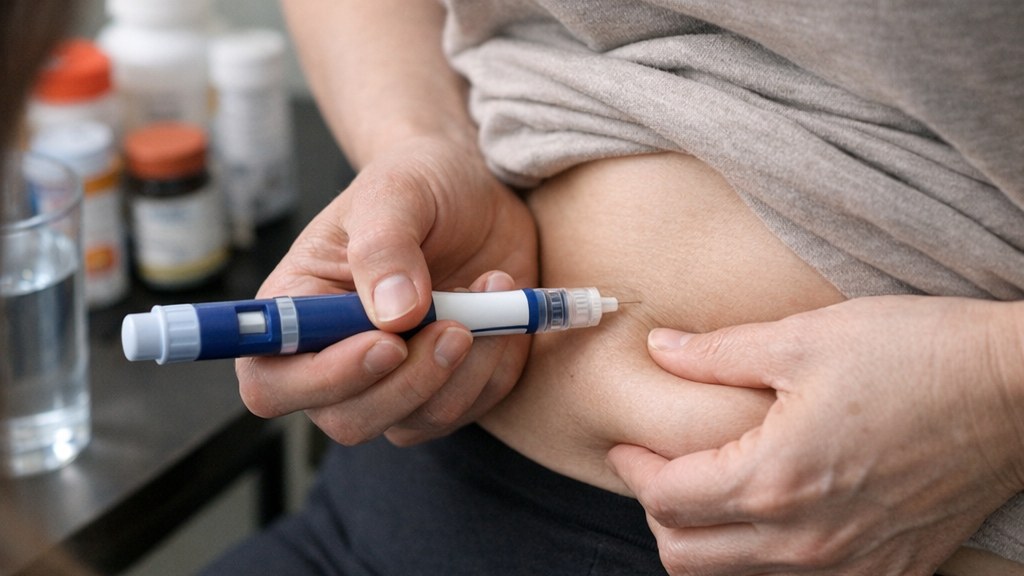
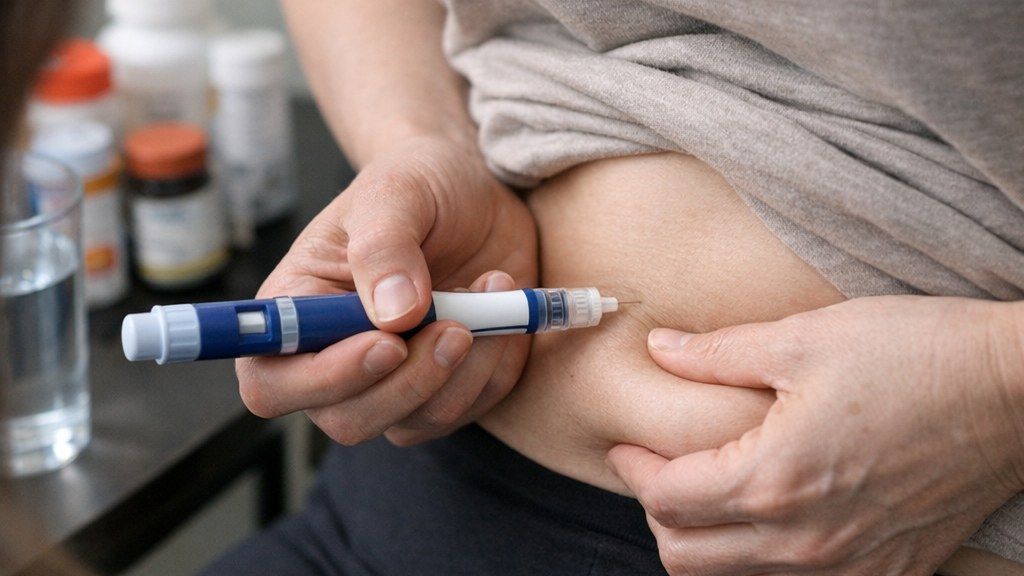
More serious risks are less common but important. Labels warn about pancreatitis, gallbladder disease, possible kidney injury linked to dehydration and serious allergic reactions. GLP-1 drugs can delay stomach emptying, which can matter before surgery or procedures using anesthesia or deep sedation.
Some medicines also carry warnings related to thyroid C-cell tumors seen in animal studies. They are not recommended for people with a personal or family history of medullary thyroid cancer or for people with multiple endocrine neoplasia syndrome type 2.
Cost is another major barrier. Many patients face uneven insurance coverage, prior authorization rules or high out-of-pocket prices. Medicaid coverage for obesity-only use remains limited in many states, and employer plans vary widely.
High demand has also fueled a market for compounded or otherwise unapproved versions. Federal regulators have warned that unapproved semaglutide and tirzepatide products are not reviewed for safety, effectiveness or quality in the same way as approved medicines. Reports of dosing errors and adverse events have added to those concerns.
## The unknowns: what happens after years of use
The biggest unanswered questions are long term. Obesity is a chronic condition, and many patients regain weight after stopping treatment. Researchers are still studying the best way to maintain results, whether some people can safely taper off and how to manage treatment over many years.
Body composition is another open question. Weight loss can include fat and lean mass. Doctors often advise resistance training and enough protein to help protect muscle, but the best monitoring strategy is still being studied.
There are also broader questions about who benefits most, who is at higher risk of side effects and how these medicines should be used in people with complex medical histories. The field is advancing fast, but the science is still catching up with public demand.
For now, medical groups generally treat GLP-1 drugs as powerful tools, not quick fixes. They work best when prescribed for appropriate patients and combined with long-term care, nutrition support and physical activity.
AI Perspective
GLP-1 drugs show how fast biotechnology can change everyday medicine. Their promise is real, but so are the limits around cost, safety monitoring and long-term use. The most balanced view is to see them as medical treatments that need careful prescribing, not as simple lifestyle shortcuts.































































-b9c5792e.jpeg)













-dce9c62e.jpeg)