[[[SUMMARY_START]]]
New research is sharpening the picture of how psilocybin may produce effects that outlast the drug’s brief presence in the body.
Recent animal studies point to activation of the serotonin 5-HT2A receptor in key frontal brain cells as a driver of persistent structural changes.
The findings add support to the idea that brief psychedelic exposure can trigger longer-lasting neural plasticity, while also showing the biology is more complex than one receptor alone.
[[[SUMMARY_END]]]
A growing body of research suggests that psilocybin may leave a longer mark on the brain than its short-lived psychedelic effects would imply. Newer studies in mice are linking that durability to activation of the serotonin 5-HT2A receptor, especially in specific frontal-cortex neurons, and to structural changes such as growth and remodeling at synaptic connections.
Scientists have been trying to answer a basic question about psilocybin for years: how can a drug that clears the body within hours be associated with effects that may last for days, weeks, or longer?One leading explanation is neural plasticity. That term describes the brain’s ability to rewire itself by strengthening, weakening, or reshaping connections between nerve cells. In the case of psilocybin, researchers have focused on whether a short burst of receptor activity can set off a longer biological chain reaction.
## A receptor long seen as central
The main receptor in that discussion is 5-HT2A, a serotonin receptor already known to play a central role in the acute psychedelic experience. Recent work has pushed the story further by connecting that same receptor to enduring structural changes in the brain.
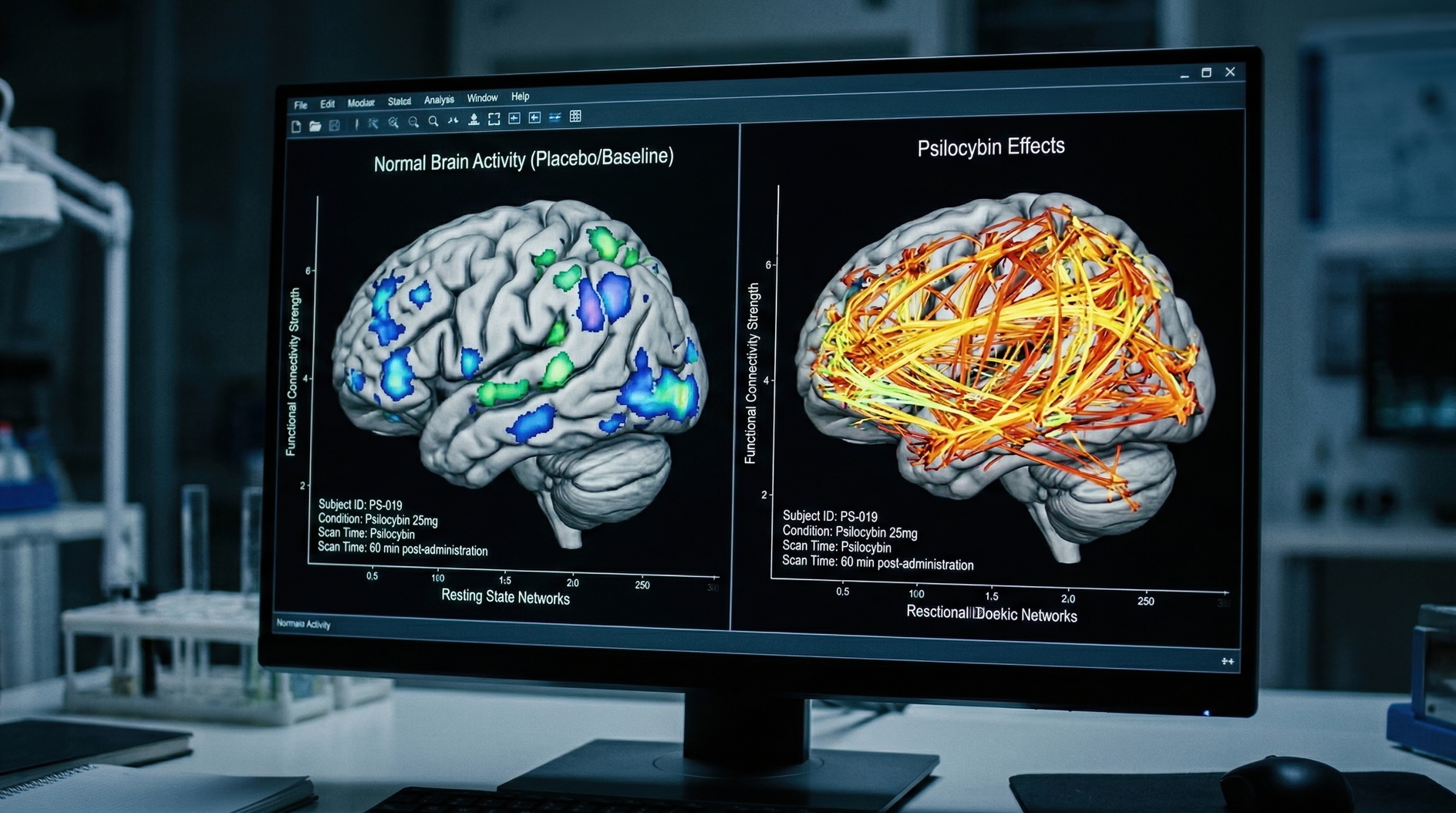
In a 2025 study published in *Nature*, researchers found that psilocybin’s longer-term actions in mice depended on 5-HT2A receptors in the medial frontal cortex, a brain region involved in mood, decision-making, and cognitive control. The team reported that removing those receptors from targeted neurons blocked psilocybin-driven structural plasticity and also prevented key longer-lasting behavioral effects seen in stress-related models.
The study also narrowed the mechanism to a particular class of excitatory brain cells called pyramidal tract neurons. After psilocybin exposure, those neurons showed stronger activity and structural remodeling at dendritic spines, the tiny protrusions that help neurons form synaptic connections. Those spine changes are widely used as a marker of altered circuit structure.
## Why structural change matters
This matters because structural plasticity offers a plausible bridge between a short drug exposure and a sustained biological response. If synapses are physically reshaped, brain circuits may not return immediately to their earlier state after the compound is metabolized.
That does not mean scientists now have a complete map of psilocybin’s action. Other recent work suggests the picture is broader. A 2026 study in *Molecular Psychiatry* found that the serotonin 1B receptor also contributed to some of psilocybin’s longer-lasting behavioral effects in mice. In that study, removing or reducing 5-HT1B signaling changed some persistent responses even though the classic acute head-twitch response, often used as a marker of 5-HT2A activation in rodents, remained intact.
Taken together, the findings suggest that 5-HT2A receptor activation is a key trigger for structural brain changes, but it may not be the only pathway shaping longer-term outcomes.
The work is drawing attention because psilocybin is being studied as a possible treatment for disorders including depression and some forms of anxiety. Researchers have long suspected that its therapeutic promise could rest not only on the immediate subjective experience, but also on a temporary opening for brain circuits to reorganize.
Animal findings fit that idea. Earlier preclinical studies had already shown increases in dendritic spine density, synaptic markers, and other signs of plasticity after psilocybin or related psychedelics. The newer papers add more precise detail by identifying which cell types and receptor systems appear to be required for at least some of those durable effects.
That could matter for drug development. If researchers can separate the biology tied to therapeutic plasticity from the biology tied to hallucinations, it may be possible to design future compounds that keep some benefits while reducing unwanted effects. But that goal remains experimental.
## Important limits
The latest findings are important, but they should be read carefully. Much of the strongest mechanistic evidence so far comes from mice, not humans. Structural changes in rodent frontal cortex do not automatically translate into safe or effective treatments for people.
Human brain imaging studies have shown that psilocybin can rapidly alter large-scale brain activity and connectivity. But proving lasting structural remodeling in living human brains is harder than tracking such changes in animal models with direct microscopy and genetic tools.
Researchers also caution that the term “lasting” in these studies does not always mean permanent. In many experiments, it refers to changes that persist well beyond the acute drug window, not necessarily lifelong alterations.
Even so, the new work marks a significant step in a field that is moving from broad observation to specific mechanism. Instead of simply saying psilocybin changes the brain, scientists are beginning to identify which receptors, which cells, and which forms of plasticity may explain why some effects endure after the trip ends.
AI Perspective
This research shows how psychedelic science is becoming more precise. The big shift is from asking whether psilocybin changes the brain to asking exactly how, where, and through which receptors those changes happen. That kind of detail is likely to shape the next generation of mental health drug research.



























































-b9c5792e.jpeg)













-dce9c62e.jpeg)

-e1b592cb.jpeg)
-ce4b953e.jpeg)
-40207ced.jpeg)